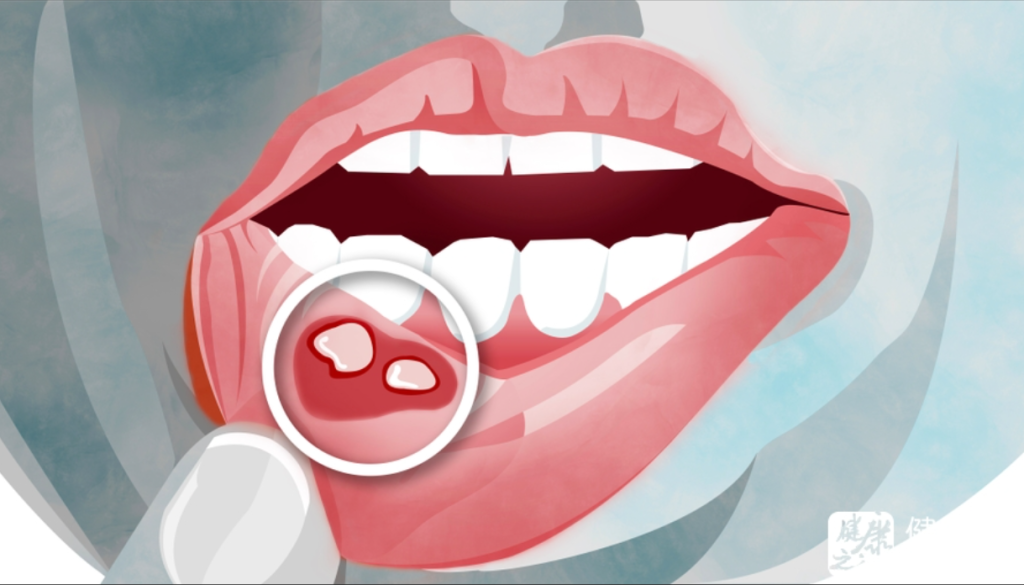
Mouth ulcers, also known as canker sores or canker sores, are small, painful sores that form inside the mouth. They can occur on the tongue, inner cheeks, gums, or palate. While they are usually harmless and tend to heal on their own within a week or two, they can cause discomfort and make it difficult to eat or speak.
By providing a comprehensive overview of mouth ulcers, this article aims to empower readers with the knowledge to recognize, manage, and prevent this common oral condition. Whether you are looking for relief from the discomfort of an existing ulcer or want to prevent it from occurring, this article will provide an invaluable resource for effectively understanding and managing mouth ulcers.
Causes of Mouth Ulcers
Mouth ulcers are a common oral condition that affects a large portion of the population. The prevalence tends to be higher in certain groups, such as adolescents and young adults.
Several factors can contribute to the development of mouth ulcers. The exact cause may vary from person to person, but some common triggers and factors include
Injuries: Accidental bites to the cheek or tongue, dental procedures, or aggressive brushing can lead to tissue damage that can cause ulcers to form.
Specific foods: Studies have shown that spicy or acidic foods, such as citrus fruits, tomatoes, or chocolate, can irritate delicate tissues in the mouth and trigger ulcers in susceptible individuals.
Hormonal changes: Some people may develop mouth ulcers during hormonal fluctuations, such as menstruation.
Stress and anxiety: Emotional stress and anxiety can weaken the immune system, making the body more susceptible to mouth ulcers, as described in this study.
Nutritional deficiencies: Deficiencies in essential nutrients, such as vitamin B12, iron and folic acid, can lead to the development of canker sores.
Autoimmune diseases: Certain autoimmune diseases, such as behaperet disease or celiac disease, are associated with a high risk of recurrent mouth ulcers.
Infections: Viral or bacterial infections, such as herpes simplex virus (HSV) or thrush (caused by Candida), can lead to the formation of mouth ulcers.
Genetic susceptibility: Some people may have a genetic predisposition to developing mouth ulcers, making them more likely to occur.
Types of mouth ulcers
1. Mouth ulcers (canker sores)
Symptoms and Characteristics
Small, round or oval sores with white or yellowish centers and red edges.
Pain or discomfort, especially when eating or drinking
Pressure or burning sensation at the site of the ulcer.
Usually heals within 1 to 2 weeks without scarring.
Triggers and Risk Factors
Minor oral injuries, such as accidental bites or hard brushing.
Certain foods, including citrus fruits, spicy or salty foods, and chocolate.
Hormonal changes, stress or emotional factors.
Nutritional deficiencies, such as iron, vitamin B12 or folic acid.
Family history of mouth ulcers.
Treatment options and self-care tips
Over-the-counter topical gels or ointments that reduce pain and promote healing.
Prescription mouthwash or corticosteroid preparations may be used in severe cases.
Avoid allergic foods and maintain good oral hygiene.
Use a soft-bristled toothbrush and practice gentle brushing.
Rinsing your mouth with a salt water or baking soda solution can provide temporary relief.
Use ice or over-the-counter anesthetic gels to relieve pain.
2 Herpes labialis (herpes simplex virus type 1)
Symptoms and transmission
Fluid-filled blisters or sores that appear on or around the lips, mouth, or nose.
A tingling or burning sensation precedes the appearance of the blisters.
According to research, herpes labialis is highly contagious and can be spread through direct contact, such as kissing or sharing utensils.
Factors that trigger outbreaks
Stress, fatigue or emotional disturbances
Exposure to sunlight or ultraviolet rays.
A weakened immune system due to illness or medication.
Menstrual or hormonal changes.
Trauma: Trauma or injury to the affected area
Medical treatment and home remedies
Antiviral medications (prescription or over-the-counter) to reduce the severity and duration of the outbreak.
Topical creams or ointments to reduce pain and promote healing.
Avoiding triggers, such as prolonged exposure to sunlight or stress.
Use cold or ice packs to reduce pain and swelling.
Keep the affected area clean and avoid touching or scratching the sore.
Use over-the-counter lip balm and sunscreen to protect against UV rays.
3 Thrush (Candidiasis)
Causes and Risk Factors
Overgrowth of Candida (usually Candida albicans) in the mouth.
A weakened immune system, such as in people with HIV/AIDS or those undergoing chemotherapy.
Antibiotic use disrupts the natural balance of oral microorganisms.
Poor oral hygiene.
Poorly fitting dentures or dental appliances.
Symptoms and complications
Milky white lesions on the tongue, inner cheeks, gums or throat.
Redness or pain in the affected area.
Difficulty swallowing or changes in taste.
In severe cases, the infection may spread to the esophagus.
Treatment options and preventive measures
Antifungal medications (oral or topical) to eliminate the Candida fungus.
Maintain good oral hygiene, including regular brushing and flossing.
Remove and clean dentures properly.
Avoid excessive sugar intake.
Seek treatment for underlying conditions that weaken the immune system.
Rinse mouth with salt water or diluted hydrogen peroxide to relieve symptoms.
Summary
Mouth ulcers come in different forms, including canker sores, herpes labialis, and thrush. Mouth ulcers are small, painful sores that heal in a week or two. They can be triggered by trauma, certain foods, hormonal changes and stress. Treatment includes topical gels, mouthwash and avoiding triggers. Herpes labialis, caused by the herpes simplex virus, presents as fluid-filled blisters and is contagious. Outbreaks may be caused by stress, sunlight or a weakened immune system. Antiviral medications, creams and home remedies can help treat herpes labialis. Thrush is a fungal infection characterized by white lesions. Antifungal medications, good oral hygiene and addressing the underlying problem are key to treatment and prevention.
Possible Complications of Untreated Mouth Ulcers
Untreated mouth ulcers can lead to a variety of complications, including
Infection: If an ulcer becomes infected, it can lead to a more serious and longer healing process.
Constant pain: Some ulcers may not heal in the expected time frame, leading to prolonged pain and discomfort.
Difficulty eating and speaking: Large or multiple ulcers can make it difficult for you to eat, drink or speak properly.
Scarring: In some cases, especially deeper or severe ulcers, scarring may occur after healing, leading to long-term tissue damage.
Signs of needing immediate medical attention
While most mouth ulcers will heal on their own without medication intervention, certain signs may indicate the need for urgent care. Seek immediate medical attention if you experience any of the following.
Prolonged duration: If the ulcer shows no sign of improvement after two weeks, or if the ulcer has persisted for a long time.
Severe pain: If the pain is severe and is not relieved by over-the-counter pain medications or home remedies.
Excessive swelling: Unusual swelling can affect your ability to eat or breathe.
High fever: If you have a high fever along with an ulcer, this may indicate an underlying infection.
Difficulty swallowing or breathing: If the ulcer is causing severe difficulty swallowing or breathing, seek medical help immediately.
Spreading or worsening symptoms: If the ulcer is spreading rapidly or if symptoms are worsening despite self-care measures.
It is important to note that these signs may indicate a more serious underlying disease or infection that requires prompt medical attention. If you are unsure or concerned about your mouth ulcers, it is best to consult a healthcare professional for an accurate diagnosis and appropriate treatment.
Prevention Strategies for Mouth Ulcers
1. Lifestyle changes to reduce the risk of developing mouth ulcers
Get enough sleep: Prioritize quality sleep to support a strong immune system and overall health.
Practice gentle oral habits: Avoid habits such as nail biting, pen biting, or using sharp objects in the mouth that can cause mouth damage.
Manage stress: Engage in stress-reducing activities such as exercise, meditation or yoga to reduce stress levels that can weaken the immune system.
Quit Smoking: Smoking irritates the mouth and increases the risk of developing mouth ulcers. Quitting smoking is good for overall oral health.
Limit alcohol consumption: Excessive alcohol consumption can irritate the oral mucosa. Moderation is the key to reducing the risk of ulcers.
2 Maintain good oral hygiene habits
Brush your teeth often: Brush your teeth at least twice a day with a soft-bristled toothbrush and fluoride toothpaste. Good oral hygiene helps prevent oral infections.
Floss daily: Use dental floss or a gap cleaner to clean between your teeth to remove food particles and plaque.
Replace your toothbrush: Replace your toothbrush every three to four months, or sooner if the bristles are worn out.
Visit the Dentist: Regular dental checkups allow for early detection and treatment of oral health problems.
Use mouthwash: Rinsing your mouth with an antibacterial mouthwash can help reduce oral bacteria and keep your mouth healthy.
3 Dietary modifications and avoidance of triggers
Avoid foods that cause canker sores: Identify and avoid foods that cause canker sores. Common triggers include spicy, acidic or rough foods.
Maintain a balanced diet: Eat a nutritious diet rich in vitamins, minerals and antioxidants to support overall oral health.
Stay hydrated: Drink plenty of water to keep your mouth moist and prevent dryness, which can lead to ulcers.
Watch out for dental injuries: Be careful when eating to avoid accidentally biting your tongue, cheek or lip.
Use protective equipment: Use an appropriate mouth guard or protective equipment if participating in sports or activities that could lead to oral injuries.
Recommendations:
Mouth ulcers can occur frequently if you eat a lot of spicy or acidic foods or have a tendency to bite the inside of your cheeks or lips. While this can be painful, these do go away quickly. In the meantime, don’t eat foods that are too hot, spicy, or acidic, and don’t repeatedly lick the sore spot with your tongue.
Conclusion
Mouth ulcers can be a bothersome condition, but the likelihood of them occurring can be minimized with proper understanding and preventative measures. By maintaining good oral hygiene, modifying diet, and avoiding triggers, individuals can reduce their risk of developing ulcers. Prompt treatment and self-care strategies can help relieve symptoms and promote healing. However, it is important to seek medical attention if complications arise or emergency symptoms develop. Through proactive oral health and timely intervention, individuals can effectively manage their canker sores and improve their quality of life. Remember to consult a healthcare professional for personalized advice and guidance tailored to your specific situation.
Disclaimer: The purpose of this article is only to disseminate knowledge and raise awareness. It is not intended to replace the medical advice of a professional. For more information, please contact your doctor.
Frequently Asked Questions (FAQs)
Q: What are the causes of mouth ulcers?
Mouth ulcers can be caused by a variety of factors such as injury or trauma to the oral cavity, certain foods or beverages that irritate the mucous membranes of the mouth, hormonal changes, stress, nutritional deficiencies, autoimmune disorders, infections and genetic susceptibility.
Q: How are mouth ulcers treated?
Treatment of mouth ulcers usually focuses on relieving symptoms and promoting healing. Over-the-counter topical gels or ointments can relieve pain. Rinsing with a salt water or baking soda solution can help relieve ulcers. In severe cases, healthcare professionals may prescribe mouthwash, corticosteroids or other medications to reduce inflammation and promote healing.
Q: Why do mouth ulcers occur?
The exact cause of mouth ulcers varies from person to person. They can be triggered by injury, certain foods, hormonal changes, stress, nutritional deficiencies, immune system disorders, infections, or genetic factors. Understanding the underlying causes can help manage and prevent their occurrence.
Q: How can I get rid of canker sores quickly?
While there is no guaranteed way to get rid of a canker sore overnight, there are steps you can take to promote faster healing. These include maintaining good oral hygiene, avoiding spicy or acidic foods, using over-the-counter topical gels or ointments for pain relief, and rinsing your mouth with salt water or baking soda solution to keep it clean. However, it is important to note that individual healing times may vary.
Q: What are the causes of mouth ulcers?
Mouth ulcers can have a variety of causes, including oral injuries or trauma, certain foods or beverages that irritate the mucous membranes of the mouth, hormonal changes, stress, nutritional deficiencies, autoimmune disorders, infections, or genetic factors. Determining the specific cause of mouth ulcers may require medical evaluation.
Q: How can I heal a canker sore in one day?
Unfortunately, there is no guaranteed way to heal canker sores in one day. Most canker sores heal on their own within one to two weeks. However, you can help relieve symptoms and promote healing by using over-the-counter topical gels or ointments, maintaining good oral hygiene, avoiding irritants, and rinsing with a salt water or baking soda solution. If you have concerns or the ulcer persists, it is recommended that you consult a healthcare professional for proper evaluation and guidance.